 In the LIVE trial, patients were randomized to standard of care or personalized mechanical ventilation. ĭistinct lung morphological patterns, namely focal, diffuse and patchy (the last two together are also called non-focal), have been identified in the early 2000s through physician-driven pattern recognition. 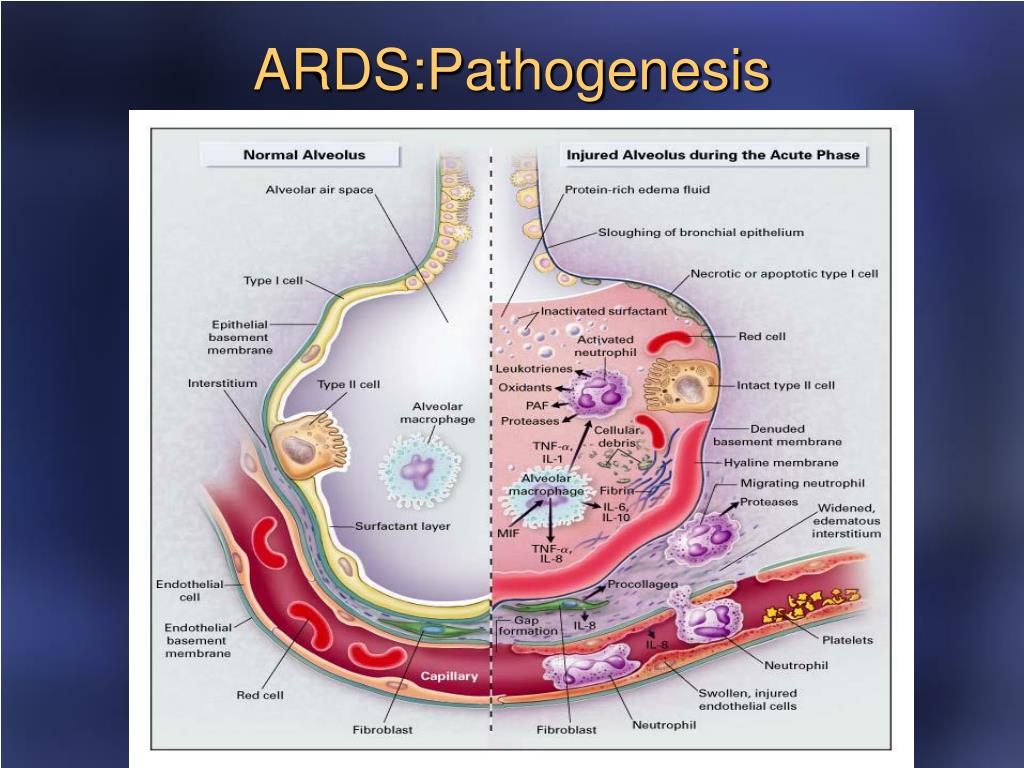
The main limitation of this approach is that plasma biomarkers do not necessarily reflect pulmonary disease in critically ill patients with multiple organ failure and indeed these phenotypes could also be recognized in patients without ARDS. These hallmark studies have shown that ARDS can be repeatedly and reliably sliced into more homogenous portions. Importantly, systemic inflammatory phenotypes showed differential responses to positive end-expiratory pressure (PEEP) strategy, fluid strategy and administration of simvastatin. proposed ARDS phenotypes based on latent class analysis (LCA) of a combination of plasma biomarkers and clinical characteristics and found that mortality was higher in the ‘hyper-inflammatory’ than in the ‘hypo-inflammatory’ phenotype (prognostic enrichment). The promise of precision medicine is that outcomes can be improved through the identification of homogeneous groups (the so-called ARDS phenotypes) that do benefit from a specific treatment. 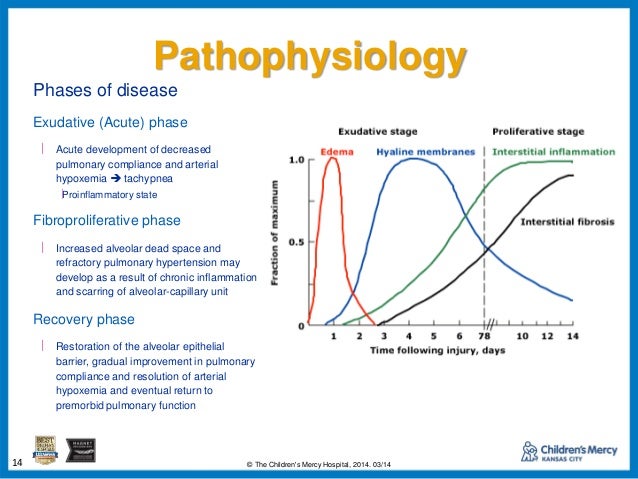 .jpg)
Considerable etiological, physiological and biological heterogeneity is apparent in patients with ARDS, which has likely hampered clinical trials to show benefit of treatment strategies. The acute respiratory distress syndrome (ARDS) is a critical illness characterized by severe lung inflammation and pulmonary oedema caused by increased alveolar permeability. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
